How Bacteria Build Resistance at the Cellular Level
Antibiotic resistance is a complicated issue. You may be aware that it is one of the greatest threats to public health, but maybe you’re less clear on what exactly it means. MPH@GW worked with The Antibiotic Resistance Action Center (ARAC) at the Milken Institute School of Public Health at the George Washington University to create a series of graphics that illustrates the interaction between antibiotics and bacterial cells within your body — because bacterial cells, not people, become resistant to antibiotics. The following graphics are intended to help explain what happens at the cellular level. To learn more about antibiotic resistance and the rise of “superbugs,” check out the work being done by ARAC.
4 Ways Antibiotics Affect Bacterial Cells
The first graphic depicts different ways that antibiotics can affect bacterial cells when antibiotics work correctly. Antibiotics are used to treat bacterial infections by destroying the bacteria themselves or preventing their growth. It is important to keep in mind that antibiotics are designed to destroy bacteria, not viruses. Attempts to use antibiotics to treat a viral infection will be ineffective. However, this inappropriate use could expose bacteria to subtherapeutic doses of antibiotic, favoring the growth of resistant bacteria.
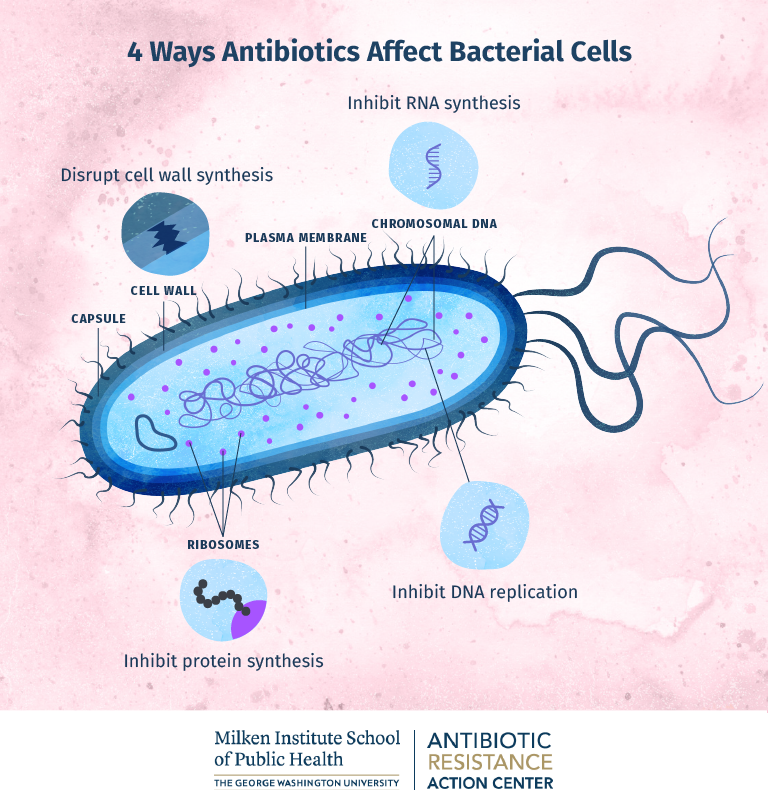
Mechanisms of Antibiotic Resistance
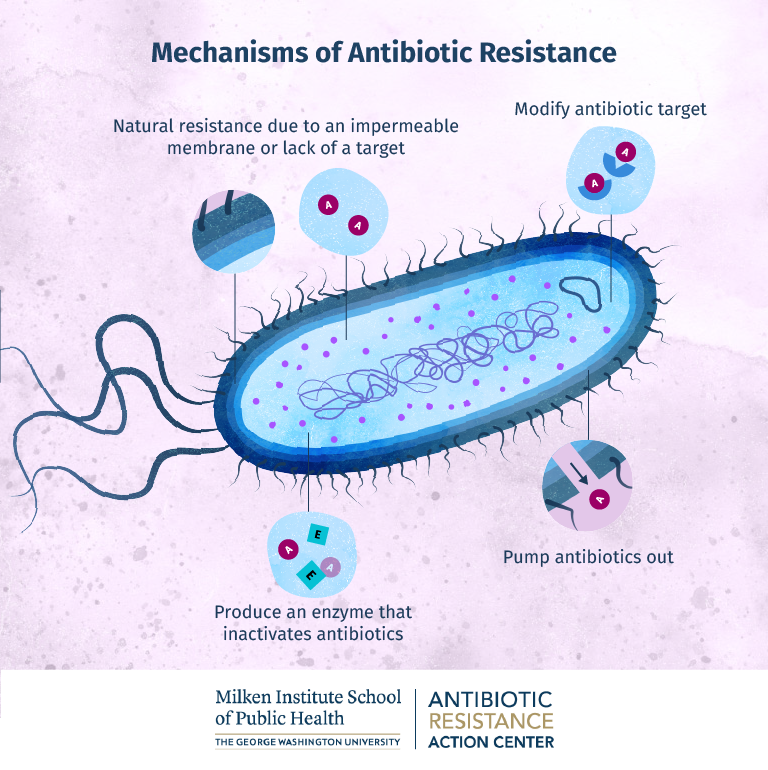
There are a number of mechanisms that bacterial cells use to thwart the efforts of antibiotics. Some bacteria are naturally resistant due to an unusually impermeable cell membrane or a lack of the target that the antibiotic attacks. Other bacteria are capable of producing enzymes that can inactivate antibiotics upon contact. In some cases, bacteria can modify the antibiotic’s target, rendering the antibiotic ineffective. Bacteria can also produce efflux pumps, which can transport antibiotics out of the bacterial cell before they can take effect.
Ways that Bacteria Acquire Resistance
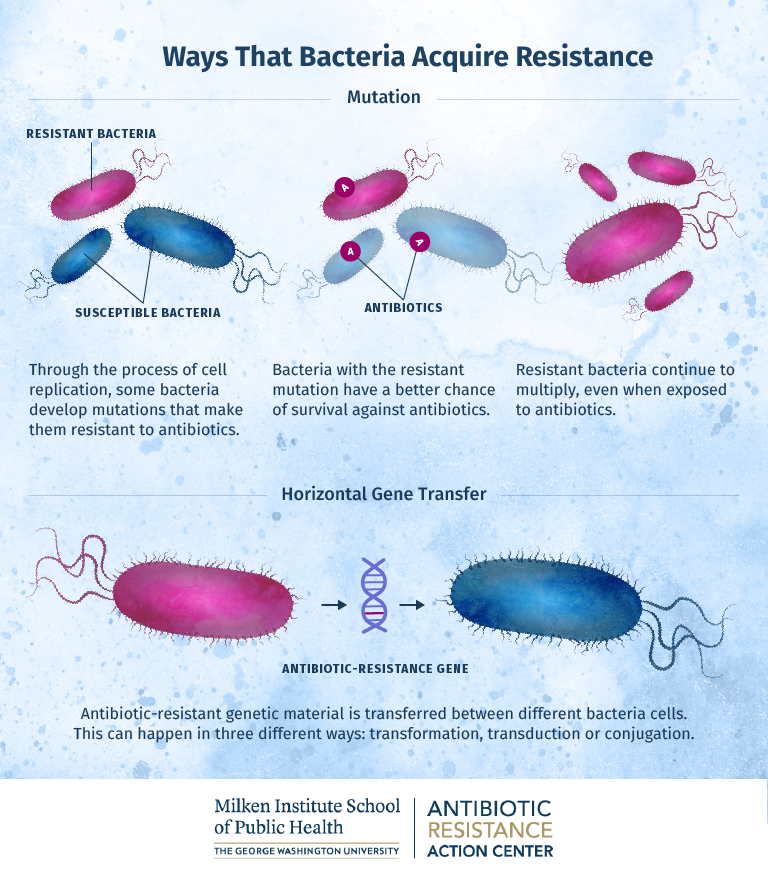
There are two main ways that bacterial cells can acquire antibiotic resistance. One is through mutations that occur in the DNA of the cell during replication. The other way that bacteria acquire resistance is through horizontal gene transfer. There are three different ways in which this can occur, but in each case genetic material is transferred from antibiotic-resistant bacteria to other bacterial cells, making them resistant to antibiotics as well. Once bacterial cells acquire resistance, exposure to antibiotics kills off non-resistance bacteria, while the antibiotic-resistant bacteria proliferate.
To learn more about antibiotic resistance, check out The Antibiotic Resistance Action Center.
ARAC was created to preserve the effectiveness of antibiotics by engaging in research, advocacy and science-based policy. Follow ARAC on Twitter, Facebook and Instagram.


